


University of the Sciences in Philadelphia. S. Ayitos, MD: "Buy cheap Sumatriptan online - Trusted Sumatriptan online OTC".
In asymptomatic older patients order 50 mg sumatriptan fast delivery spasms quadriplegic, output and pressures are usually normal except for a slight increase in left ventricular end-diastolic pressure buy sumatriptan 25mg xanax muscle relaxer. There may be a left-to-right shunt at the pulmonary arterial level buy sumatriptan on line amex spasms pelvic area, but because the shunt may be small, its absence does not rule out the diagnosis. Aortic root angiography will show the dilated right coronary artery and, if there are large collaterals, will show filling of the left coronary artery and passage of contrast material from the left coronary to the main pulmonary artery. Attempts at selective left coronary artery angiography will only show filling of the left sinus of Valsalva without opacification of the left coronary artery. Usually selective right coronary artery angiography is diagnostic in showing filing of the left coronary artery via collaterals, with backfilling to its pulmonary ostia (see Video 32. Although pulmonary arterial angiography may show reflux of contrast medium into the origin of the left coronary artery, neither this nor left ventriculography can reliably make the diagnosis. Natural History Of all children born with this rare anomaly, approximately 87% present in infancy (33) and of these, 65% to 85% die before 1 year of age from intractable congestive heart failure (37), usually after 2 months of age. Others never have symptoms, perhaps because of extensive collaterals and even a restrictive opening between the origin of the left coronary artery and the pulmonary trunk. Nevertheless, even these people are at high risk of sudden death (35), especially during exercise. Some present as adults with exercise-induced angina (34) or with congestive heart failure owing to mitral regurgitation (18). Treatment The first effective surgical treatment was ligation of the left coronary artery at its origin from the pulmonary artery to prevent the steal. Most older children benefit from this procedure, especially if they have extensive coronary- to-pulmonary arterial shunting, but late sudden death can still occur (34,39). Ligation of the origin of the left coronary artery and revascularization via an internal mammary arterial or saphenous venous graft has been successful (40,41), although graft thrombosis and stenosis has occurred, to a much greater degree with vein grafts. Grafts using the internal mammary artery have a longer survival and are preferred when coronary reimplantation cannot be done. Direct reimplantation of the origin of the left coronary artery into the aorta (with a button of pulmonary artery around the origin) has been proven successful and is considered the standard approach in many centers (42,43,44,45). An alternative approach is the Takeuchi procedure, in which an aortopulmonary window is created and then a tunnel fashioned that directs blood from the aorta to the left coronary ostium (46). In the past it was recommended that, because surgical mortality is high in the sickest infants, surgery should be delayed until after 18 to 24 months of age (47). More recently, as surgical experience has accrued, early surgical intervention to establish a two-coronary system has been found to have significantly improved outcomes (45,48). Additionally, it has been reported that a two-vessel repair is feasible even in the sickest infants if postoperative support with a left ventricular assist device is used (49). Coronary Artery Fistulae Coronary fistulae are persistent and abnormal connection between the coronary artery and one of the cardiac chambers or pulmonary arteries. In the modern era of high-resolution ultrasound imaging, they are frequently discovered incidentally and if small, pose no significant burden to the patient. However, less commonly they may be large and impose a significant hemodynamic burden or future risk for cardiovascular events (Video 32. Embryologic Development Coronary artery fistulae connecting to the intracardiac chambers are likely the sequelae of incomplete reabsorption of myocardial trabeculations as they connect to the nascent coronary arteries. It has been hypothesized that fistulae connecting to the pulmonary artery may be a consequence of the failure of involution of the aortopulmonary anlage (50). Pathophysiology There are three pathophysiologic consequences of a significant coronary fistula: 1. Distal coronary insufficiency While the presence of any of these findings warrants intervention, it is also clear that coronary fistula may develop significance over time. Some small- to moderate-sized coronary fistulae have demonstrated the capacity to grow over time, while other small ones remain trivial. It is not clear what the risk factors are for development of pathologic significance in such small fistulae. Imaging Most commonly, small coronary fistulae are picked up on echocardiography as a small shunt seen in diastole from the myocardium to a low-pressure right-sided chamber. In these cases, left-sided chambers are of normal dimensions indicating that the degree of shunting is small. It is unusual for there to be an audible murmur associated with small coronary fistulae. Large coronary fistulae may be initially diagnosed following a referral for an abnormal murmur, which may be continuous. The surface echocardiogram may demonstrate dilatation of left-sided chambers, and depending on where the fistula enters the right heart, the right-sided chambers as well. In such large fistulae, the proximal coronary anatomy on the side of the fistula is markedly dilated and may be seen by echocardiography (Video 32. In the older patient, cardiac computed tomography usually provides excellent delineation of the location and anatomy of the large fistula, albeit at a significant radiation dose. Its utility in the younger pediatric patient is limited by tachycardia-created motion artifact. Similarly cardiac magnetic resonance imaging has value in the older patient to determine both the anatomy of the fistulous connection as well as quantifying the degree of associated chamber enlargement. Coronary angiography provides the gold standard for diagnosis and anatomic delineation as well as determination of hemodynamic burden for coronary fistulae (Video 32. It is indicated in patients in whom pathophysiologic burden is identified or suspected by noninvasive imaging, and in those undergoing planned intervention. Therapeutic Interventions As previously cited, therapeutic interventions on coronary fistulae are indicated for those with pathophysiologic burden to the fistula. It is controversial whether intervention on small- to moderate-sized fistulae are indicated to prevent their growth into a larger shunt; given the potential risks associated with coronary fistula intervention, the authors do not recommend intervention in the absence of documented physiologic burden. Interventions on coronary fistulae include transcatheter occlusion and open surgical ligation. Due to the persistence of coronary microvascular dysfunction after fistulae therapy, after either approach long-term follow- up is warranted. This usually involves delineation of the fistula anatomy from a retrograde transarterial approach, to define the “neck” of the fistula proximal to it entering the right-sided chamber or pulmonary artery. Care must be exercised not to compromise circulation to viable myocardial territory. The occluding coil or plug then can be delivered from either the aortic side, or a through- and-through wire rail can be achieved to allow a plug to be delivered from the right-heart side (Video 32. Frequently, follow-up imaging will demonstrate dramatic reduction in the intraluminal proximal coronary size (Video 32. However, it should be noted that this does not mean that the vessel is “normal,” and should warrant follow-up as well as recommendations for life-long healthy habits to prevent atherosclerosis. Rare Coronary Anomalies Coronary Atresia Total absence of the extramural coronary arteries is very rare and occurs most often with either pulmonary atresia or aortic atresia. In both these anomalies, pressure in the small but hypertrophied right or left ventricle is at or above aortic pressure, and enlarged sinusoids carry blood from the ventricle to be distributed in the distal coronary arterial branches. Stenosis or Atresia of a Coronary Ostium Stenosis or atresia of the ostium or first few millimeters of the left main coronary artery is one of the rarest of the congenital coronary anomalies.
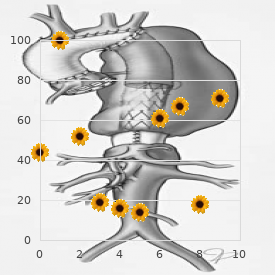
It is not known if the mecha- Blunt Injury nismofinjuryaftersuchalocalizedinsultisdiferentor Four patients presented with traumatic optic neuropathy whether the delayed presentation may have also contrib- after blunt trauma (usually a motor vehicle accident) buy cheapest sumatriptan spasms stomach. Two patients had an obvious fracture through the bony Results of Optic Nerve Decompression optic canal (Fig order 25 mg sumatriptan otc spasms throat. Four patients presented with compressive lesions of the The third patient improved from light perception to 6/60 vi- orbital apex or optic canal with progressive visual loss discount 25 mg sumatriptan with amex muscle relaxant before massage. Three of these patients were left with lim- extended signifcantly into the bony optic nerve canal. This patient presented with progressive visual loss and 15 Endoscopic Optic Nerve Decompression 197 Fig. Postoperatively she regained normal vision which of his orbital apex and optic canal. This again tients with long-term visual loss may not respond as well as improved her vision to 6/18 without further deterioration patients who present with more rapid visual loss due to optic (Fig. The second patient presented with an 8-month progres- Two patients with compressive lesions (lateral sphe- sive visual loss and at presentation could only see hand noid wing meningioma and an encircling fibrous dys- Fig. The compressive lesion on the orbital apex and optic canal is indicated by the white arrows. Injudicious use of inappropriate instruments has the potential to worsen the vision and this should be kept in mind during the procedure. Transethmoidal optic nerve contemplated unless there is an obvious bony fragment decompression. Endo- series presented in this chapter and from larger studies in scopic optic nerve decompression for traumatic blindness. Otolaryngol 1–4,10 Head Neck Surg 2000;123(1 Pt 1):34–37 the literature suggest that patients should be operated 3. Powered instrumentation in orbital and optic nerve mol 1994;38(6):487–518 decompression. Vasculature and morphometry of the the comatose and conscious patients after trauma. In last 10 years, new techniques have been introduced to aid addition, this route of access does not give access to the with the resection of tumors in regions which traditionally anterior and medial compartments of the maxillary sinus. As there is only a single fulcrum mors but, as techniques and adjuvant therapy develop, these around which the blade rotates, good access is provided to techniques will be increasingly applied to the resection of the medial and lateral walls, and the foor of the maxillary malignant tumors. Endoscopic resection of the medial maxilla is useful to access the anterior, posterior, and Endoscopic Medial Maxillectomy for Access to lateral walls of the maxillary sinus. The lateral Surgical Techniques for Access to the nasal wall and septum are infltrated with 2% lidocaine and Maxillary Sinus, Pterygopalatine Fossa, 1:80 000 adrenaline. A pterygopalatine fossa block is placed and Infratemporal Fossa via the greater palatine canal using 2 mL of lidocaine and adrenaline (see Chapter 2). This helps to reduce bleeding Canine Fossa Trephination for Access to the during the dissection of the medial wall of the maxilla and Maxillary Sinus (Videos 8 and 9) pterygopalatine fossa. The frst step in endoscopic medial maxillectomy is to Tumors that involve the medial wall, anterior foor, or an- remove the uncinate process and perform a large middle terior or anterolateral wall of the maxillary sinus cannot meatal antrostomy (Fig. The maxillary antrum is en- be accessed through a maxillary antrostomy irrespective of larged posteriorly up to the posterior wall of the maxillary how large this is made. Although this can orbital wall and allows removal of the residual medial max- be achieved through an inferior meatal puncture, place- illa without endangering the orbit. Most large tumors of the ment of a 4–mm microdebrider blade through the inferior maxillary sinus and/or pterygopalatine fossa will involve the meatal antrostomy tends to destabilize the inferior turbi- posterior ethmoids and sphenoid. This lary fap is performed and the frontal recess dissected with is because the nasal vestibule provides a fulcrum around exposure of the frontal ostium. The bulla ethmoidalis is re- which the blade is rotated, causing signifcant disruption moved and a posterior ethmoidectomy and sphenoidotomy 200 16 Endoscopic Resection of Tumors 201 A, B C Fig. The white arrow indicates the trephination port in the anterior face of the maxillary sinus. Any tumor large intranasal component of a soft nonvascular tumor, the extension into the anterior and posterior ethmoids can be tumor is debulked (Fig. If the tumor is very vascular or assessed and, if necessary, biopsies or frozen sections of the frm then it can be pushed superiorly or partially debulked. This Because of the posterior location of angiofbroma, debulking helps ensure complete tumor clearance. To perform the medial maxillectomy, the inferior tur- Turbinectomy scissors are used to cut along the crushed binate is medialized. A Tilley’s packing forceps is used to region of the inferior turbinate up to the point where the crush the turbinate just distal to the junction of the anterior turbinate inserts into the lateral nasal wall (Fig. Here the mucosal incision is turned ver- tically toward the posterior region of the maxillary sinus antrostomy. A sharp chisel is used to cut the bone under the mucosal incisions following the mucosal incision (Fig. The posterior vertical cut needs to enter the maxillary sinus adjacent to the posterior wall of the maxillary sinus and into the large antrostomy5 (Fig. Once the bone forming the medial maxillary wall is mobilized, the nasolacrimal duct will tether the bone an- teriorly and the duct will be visualized (Fig. Note the microdebrider blade that has been placed through the canine fossa trephine. Tumor can now be sinus, further resection of the anteromedial wall and frontal removed from the maxillary sinus under direct visualization. In such If additional access is required and the tumor does not attach cases a canine fossa trephine is not thought to be suitable due to the anterior wall of the maxillary sinus, a canine fossa to the small risk of seeding the tumor into the soft tissues of puncture can be performed. Although seeding is unlikely to occur, this risk is endoscope to be introduced through the anterior wall of the thought to be greater if the entry point into the maxillary sinus maxillary sinus which can be useful to access areas within the is through tumor rather than through normal mucosa. This access is achieved the required angle for dissection in difcult areas such as the by performing a hemitransfxion incision in the opposite nasal anterior wall or anterolateral region of the maxillary sinus. The instrument can then that attaches extensively to the anterior face of the maxillary be passed through the hemitransfxion incision, through the Fig. This allows the passage of a 70-degree dia- fxion incision anteriorly in the left nostril (contralateral side to the mond tipped drill (D). C, carti- right nasal cavity demonstrating the working tip of the drill passing into lage; F, fap. The mucosa giving greater access to the anterior wall of the maxillary sinus from the posterior wall of the maxillary sinus is elevated (Fig. This exposes the bone and removal of this of approach and usually allows complete access to the entire bone is necessary to expose the pterygopalatine fossa. The punch Access to the Pterygopalatine Fossa (Videos 41 and 42) is introduced into the sphenopalatine foramen and the bone anterior to the foramen removed until the posterior Access to the pterygopalatine fossa is achieved by remov- wall of the maxillary sinus is reached (Fig. In most cases removal of this bone can be done either with the punch a medial maxillectomy is unnecessary as most of the ptery- or with a 45-degree through-biting Blakesley. Bone is re- gopalatine fossa can be accessed through a large middle moved until the contents of the pterygopalatine fossa are meatal antrostomy. In addition the vidian nerve enters the posterior aspect of the fossa before moving laterally to end in the pterygopalatine ganglion which is suspended from the maxillary nerve (Fig.
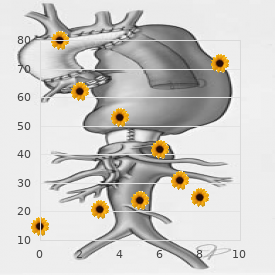
The 7- or 8-Fr sheaths are helpful when intravenous drug administration is required because a side- arm sheath larger than the catheter permits free cheap 25mg sumatriptan with amex spasms going to sleep, unobstructed flow of fluid into the vein sumatriptan 25 mg online spasms symptoms. In addition cheap sumatriptan 50 mg on-line muscle relaxant gel india, some ablation catheters have larger tips and require an 8-Fr sheath for introduction. The ultimate number and location of the sheaths also depend on the success of catheter manipulation and preference of the operator. A femoral artery cannula allows continuous monitoring of arterial blood pressure and may enhance safety, but its use is variable among laboratories. When a sheath is placed in the femoral artery for retrograde access to the left ventricle, a side-arm sheath one size larger than the catheter permits accurate pressure recordings. The use of anticoagulation to minimize thromboembolic complications also varies among laboratories and is difficult to analyze because it is difficult to separate the diagnostic procedure from the various interventional procedures (catheter ablation and the techniques used for ablation). Although there is a variety of evidence in the literature (11,12,13,14,15), none is conclusive, and practices vary from use of heparin for all procedures to use only for interventional procedures involving pulmonary venous or systemic arterial access. When used, the heparin dose varies among laboratories, but the initial dose is usually 100 U/kg, up to a maximum 5,000 to 10,000 U, depending on the expected duration of the procedure. Formerly, the 4-Fr catheters were used virtually only for infants, whereas the 5-Fr catheters most often were used in young children, and 6- and 7-Fr catheters were used for adolescents and adult-sized patients. Smaller (2 to 3 Fr) catheters can be used for intracardiac recordings as well as for right coronary artery or coronary vein epicardial mapping (16). These small catheters may be used in small children to record intracardiac electrograms throughout the conduction system. Although these small catheters may be difficult to manipulate, up to three catheters can be used in the same sheath. Traditionally, catheters used for recording and pacing were in a quadripolar configuration, whereas catheters used primarily for recording and mapping contain between 6 and 12 electrodes. Similarly, some catheters are designed to record atrial and His potentials from proximal electrodes, while distal electrodes are used to pace the ventricle. Specially formed catheters also are available for the His location with an “S”-shaped tip providing stable seating between the anterior and septal tricuspid leaflets. Short (1 to 2 mm) interelectrode distances for the bipoles, separated by 5 to 10 mm spacing allows high-quality electrograms and precise mapping, while spanning a larger region of the heart. The number of catheters used during a study depends, not only on the size of the patient and the underlying problem, but also on whether the electrophysiologist prefers the minimum or P. If the least amount of catheter manipulation is desired, a greater number of catheters are positioned initially, and these are left in place for the duration of the procedure. Electrophysiologists who use more catheters prefer the advantage of simultaneous recording from the multiple catheters to optimize data collection. If multiple changes in catheter positions are deemed acceptable, fewer catheters initially are placed. Use of fewer catheters requires moving the catheter from one area to another and perhaps back to the original position during the study. However, it may not be possible without using specialized 3-D mapping systems (described later and shown in Fig. Electrogram consistency may also be compromised or the arrhythmia affected by the catheter movement (e. Together, they provide the system by which conventional electrogram recordings are displayed, and pacing protocols are performed and recorded. A 3-D mapping system can interface with the conventional system to enhance mapping (see text) and minimize use of fluoroscopy. Integration of preprocedure cardiac magnetic resonance images or computed tomographic images can be downloaded and interfaced into the 3-D recording system. Manipulation and placement of electrode catheters involves several factors, including patient size and age, underlying arrhythmia, objectives of the individual study, size and type of catheters (e. Catheter access to the left atrium or ventricle is desirable for several reasons, usually for the purpose of recording and stimulation of the left atrium and ventricle for evaluation and mapping of supraventricular tachyarrhythmias. This has prompted use of the retrograde arterial approach or the transseptal approach via a patent foramen ovale or a transseptal needle and sheath (Brockenbrough) technique. It helps minimize the risk of perforation and enhances procedural efficiency, while maximizing the precision of catheter manipulation during mapping. For mapping, especially when it involves the tricuspid annulus, mitral annulus, and posterior septal area, the positioning of the fluoroscopy x-ray tubes in a perpendicular alignment to the long and short cardiac axes optimizes recognition of anatomic relationships (Fig. Recording and Stimulation Technique The display and recording of the intracardiac electrograms are undertaken after catheter placement. Most electrograms are displayed and recorded in a bipolar fashion, although unipolar electrograms are obtainable easily and can be helpful for mapping arrhythmia foci (17). The 3-D mapping systems, used primarily when ablation is planned, incorporate the temporal and spatial (anatomic) details and therefore provide much more precise diagnostic data (see interventional section for more details) (18). Also, most 3-D systems have the capacity to capture continuous rhythms for analysis when sustained tachyarrhythmias are not inducible or when the arrhythmia is associated with intolerable hemodynamics. The 3-D mapping systems have added an important diagnostic component to electrophysiologic studies and also have provided increased safety by decreasing radiation exposure because catheter manipulation can be performed without, or by minimizing, fluoroscopy (19,20). Regardless of the specific 3-D system used, the general characteristics are: (i) accurately replicate the cardiac anatomy underlying the arrhythmia; (ii) provide a plausible representation of activation of that chamber, as linked to the specific anatomic site of data acquisition; (iii) readily capture and intelligibly display other details of physiology; and (iv) catalog the site of interventions (18). The tricuspid valve annulus and the mitral valve annulus are depicted in positions predicted by the catheter positions to demonstrate approximate locations. The surface electrocardiographic leads and skin electrodes, as well as radiofrequency and defibrillation skin pads, are not labeled. Catheter ablation of accessory atrioventricular pathways in young patients: use of long vascular sheaths, the transseptal approach and a retrograde left posterior parallel approach. With catheters used for both recording and stimulation, the distal pair of electrodes is best for pacing consistency, and all proximal pairs are then used for recording. Because of fast tachycardia rates in children, fast recording capability (200 mm/s or higher) is essential to differentiate electrograms recorded by the various electrode catheters (Fig. The pacing and recording protocols used are variable, and emphasis should be on flexibility and patient-specific diagnosis and findings. The specific protocols chosen should be adapted to the patient as they relate to the preprocedure diagnosis, but they also should remain flexible during the study, dependent on ongoing elicited findings. It is beyond the scope of this chapter to provide examples of protocols for each specific type of arrhythmias and conduction disturbances. Most can be found either elsewhere in this chapter or in the literature (2,3,21,22,23). Also, with the advent of catheter ablation and with the advances in 3-D mapping technology, the techniques and objectives of mapping have assumed a major new role and are emphasized in the interventional section of this chapter. The important general mapping concepts include the fluoroscopic image, catheter manipulation techniques, various modes of pacing, nuances of electrogram recordings, and 3-D mapping. Administration of Drugs Intravenous drug administration during an intracardiac study encompasses three general categories: anesthetic drugs, provocative arrhythmic drugs, and antiarrhythmic drugs. Of the three, anesthetic drugs are the most commonly administered and were discussed earlier in this chapter. Other less frequently used provocative drugs include epinephrine, atropine, aminophylline, phenylephrine, procainamide, or flecainide (for Brugada syndrome) (2,3,24,25,26).
Centaurea segetum (Cornflower). Sumatriptan.
Source: http://www.rxlist.com/script/main/art.asp?articlekey=96426