


American Coastline University. A. Miguel, MD: "Purchase Seroflo online no RX - Discount Seroflo online OTC".
Overstretching of the artery is to be avoided because it leads to higher postprocedural occlusion rates cheap 250mcg seroflo with amex allergy forecast burlington vt. A 30 longer sheath has been considered to protect more against vasospasm at the level of the forearm discount seroflo online visa allergy medicine called xyzal. However order seroflo 250 mcg with visa allergy medicine rx, other studies suggest that it is the hydrophilic coating rather than the length of the sheath that 31 reduces spasms. Typical sheath dimensions used for radial access are 4F to 6F in size and 7 to 16 cm in length. Once the sheath is in place, typically 5000 units of unfractionated heparin is given as a bolus, or weight adjusted (50 units/kg), preferably intravenously to prevent postprocedural radial artery occlusion. Arterial vasospasm is a complicating factor and is prevented by adequate sedation, avoidance of limb cooling, and administration of vasodilators (eFig. Other approaches are sublingual nitroglycerin and intra-arterial (local) administration of diltiazem or nicardipine. Since the anatomic course may not be as straight, the J-tip wire and catheter should only be gently 32 advanced (eFig. Challenges in advancement can often be overcome by a Glidewire or a Runthrough coronary guidewire (both Terumo Interventional Systems). These wires tend to cannulate not only the main lumen but also side branches more easily and should be exchanged once the catheter is advanced to the brachiocephalic level. In case of radial artery or brachial artery dissection, the procedure can often still be continued because the catheter itself will serve to tamponade. Closure, however, should be documented, as with its initial recognition, with angiography using a 50/50 mix of saline and contrast material. Injection of contrast material is also useful to visualize tortuosity, which can pose major challenges not only distally but also for engagement of the ascending aorta. In these cases the catheter might need to guide the wire around the origin of the brachiocephalic artery rather than vice versa. For difficult cases, it is recommended not to lose position and to use an exchange-length 0. The use of diagnostic catheters designed for radial approaches and both coronary ostia (e. Once complete, the equipment is removed, including sheath, and a wristband with an inflatable balloon cuff is used to achieve hemostasis. To avoid thrombotic occlusion, the site is allowed to bleed back before the cuff is inflated to 2 cc over hemostasis level. Practices should have protocols that guide the deflation process and monitoring of the pulse and perfusion status. Also, the radial artery is not the best approach if larger sheath sizes are required (e. Presentation and management of complications from radial access are summarized in the postprocedural care section (see eFig. A meta-analysis of 12 studies with 5000 patients showed 33 that a radial approach was associated with a nearly 50% decrease in mortality and major bleeding risk. Percutaneous Brachial Artery Technique The brachial artery approach is similar to the femoral artery approach but rarely used, as replaced by the radial technique. Using the Seldinger method, a 4F to 6F sheath is placed into the brachial artery and flushed with 3000 to 5000 units of heparin. Proficient hemostasis after removal of the sheath is critical; the arm should be maintained straight on an arm board for 4 to 6 hours, with close observation of the radial and brachial pulses, access site, and upper arm size. The main advantage of the brachial artery for percutaneous access is the larger luminal size than the radial artery and accessibility when other access options have failed. This includes access for patients with severe peripheral arterial disease or such a degree of vascular tortuosity or body size that even with the use of extra-long coronary catheters, the coronary ostia cannot be reached. The percutaneous approach is easier than the cutdown of the brachial artery, which was in fact the first technique introduced for coronary artery catheterization by Sones and colleagues. Given the anatomic location, the access site is very close to the x-ray generator tube or image intensifier, depending on the angle. It may therefore lead to greater x-ray exposure and restriction of angiographic views. Venous Access With any concomitant procedure involving the femoral artery, the femoral vein is used most often for venous access. However, when the right-heart catheter is left in place after the procedure, the internal jugular approach is preferable (Videos 19. The internal jugular is preferred over the subclavian approach to lessen the risk for pneumothorax. Use of a micropuncture kit with a 21-gauge needle and introducer can minimize potential trauma from inadvertent puncture of the carotid artery or lung. When the jugular vein has been entered, the micropuncture assembly can be exchanged for any larger sheath (e. In addition, routine adjunctive use of portable vascular ultrasound probes can help to locate and verify the patency of the jugular vein. The femoral vein is located 1 cm medial to the femoral artery, which is the distance to be taken from the arterial pulse in the horizontal plane, and another 1 cm caudal in the vertical plane. In patients with severe tricuspid regurgitation, venous pulsations should not be mistaken for arterial pulsations. Local anesthesia and the modified Seldinger technique are applied as described earlier. The internal jugular vein is located lateral to the carotid artery access in the anatomic triangle of the two heads of the sternocleidomastoid muscle and the clavicle. For access, the patient is instructed to lie supine with the head turned 30 degrees to the contralateral side. The use of ultrasound is recommended to guide access; it has been shown to reduce the overall risk of complications by 70%, 35 carotid artery puncture in particular. A so-called high anterior approach is taken from the top of the outlined anatomic triangle, and the skin incision should not be lower than two fingerbreadths above the clavicle, to decrease the risk of pneumothorax. Under these circumstances, it is advisable to palpate the suprasternal notch and then move the finger laterally. The first hump is the medial and the second hump the lateral head of the sternocleidomastoid muscle. The inner edge of the second hump is followed in a superior direction to the 36 top of the triangle. Under local anesthesia and using the modified Seldinger technique, venous access is obtained. Access to the left atrium can be accomplished via a foramen ovale that is patent to a probe, which is the case in 20% to 30% of adults. With the tip directed medially and slightly posteriorly, the catheter is then slowly withdrawn until a slight forward and medial motion is observed into the foramen ovale. The catheter should then prolapse further into the left atrium with gentle pressure, and the position can be confirmed by the pressure waveform, blood samples demonstrating arterial saturation, or manual injection of contrast medium. If left atrial access cannot be obtained with this technique, transseptal catheterization should be undertaken. First described by Brockenbrough, Ross, and Braunwald more than half a century ago (see Classic References), transseptal catheterization more than ever has become an essential element in the current era because of the demands for the evaluation and intervention of structural heart diseases and arrhythmias (Fig.
There is involuntary inhala- tion and the airway is completely occluded by this material purchase 250 mcg seroflo overnight delivery allergy medicine that won't make you drowsy. The finding of small amounts of food material in the airway at autopsy does not indicate that the individual choked to death proven 250mcg seroflo allergy testing vhi. Approximately 20–25% of all individuals aspirate food agonally buy seroflo on line amex allergy forecast oklahoma, independent of the cause of death. Death caused by massive aspiration of food is rarely seen in a medical examiner’s office. It is most common in comatose patients who have impaired functioning of the central nervous system. The diagnosis of choking death is made at autopsy when the airway is found occluded. If the individual had an occluded airway and the object or food was removed during resuscitation, the only way to make the diagnosis would be by history. There are no specific autopsy findings indicative of choking except for occlusion of the airway. Some medical personnel will ascribe a death to choking even though the airway was never completely occluded. If laryngospasm did occur, one would expect relaxation of the larynx as the victim became agonal. Others hypothesize that a fatal “vagal reaction” or “reflex cardiac death,” mediated through the parasympathetic nervous system, occurred through hypersensitivity of the larynx to aspirated food. Mechanical Asphyxia In mechanical asphyxia, pressure on the outside of the body prevents respi- ration. Traumatic asphyxia (a term often used interchangeably with mechan- ical asphyxia) 2. Riot-crush or “human pile” deaths Traumatic Asphyxia Traumatic asphyxia occurs when a heavy weight presses down on an individ- ual’s chest or upper abdomen, making respiration impossible. One common form of Asphyxia 241 traumatic asphyxia is individuals under a car, repairing it, when the jack slips and the vehicle falls on top of them (Figure 8. At autopsy, there is con- gestion of the head, neck, and upper trunk with numerous petechiae in these areas, the sclerae, the conjunctivae and the periorbital skin. Internally, there is often no evidence of trauma in spite of the heavy weight on the chest. Individuals who survive an episode of traumatic asphyxia usually make an uneventful recovery, though occasion- ally there is some permanent visual impairment due to retinal hemorrhage. One individual who survived described a severe crushing pain and suffusion of his face followed by immediate unconsciousness. Thus, in one instance, an individual was knocked to the ground and a refrigerator and stereo were piled on top of him. An occasionally encountered form of accidental traumatic asphyxia involves individuals buried in cave-ins with their heads above the ground. The most unusual case of traumatic asphyxia seen by the authors was that of a 5-month-old infant killed by a python. The snake wrapped itself around the baby, tightening its coils whenever the child exhaled. At autopsy, the only marks on the child were teeth marks on the face where the snake had tried to swallow the child whole (his head was too big for the snake’s mouth) (Figure 8. Positional asphyxia Positional asphyxia is virtually always an accident and is associated with alcohol or drug intoxication. In this entity, individuals become trapped in restricted spaces, where, because of the position of their bodies, they cannot move out of that area or position. This results in restriction of their ability to breathe, followed by death (Figure 8. Positional asphyxia might occur if individuals fall down a well and are wedged between the walls. Every time they exhale, they slip farther and farther down the well, preventing inhalation. Riot-crush Riot-crush, as the name implies, occurs in riots, when the chest is compressed by stampeding people piling on top of each other. Traumatic Asphyxia Combined with Smothering Traumatic asphyxia combined with smothering is a combination of both these entities. An accidental form is overlay, where an infant is placed in bed for the night with either an adult or a larger child. During the night, the other individual rolled onto the infant, killing it by a combination of 242 Forensic Pathology A B Figure 8. Puncture marks on face have a semicircular configuration and are caused by the needle-like teeth of the python. Other deaths in this category are individuals buried in cave-ins, grain, or sand, etc. Rarely, a few fine petechiae of the facial skin, but not of the sclerae or conjunctivae, will be found. Burking is a combination of suffocation and traumatic asphyxia devel- oped (or at least perfected) by the “resurrectionists” Burke and Hare in the early 19th century. Victims, usually intoxicated, were brought to the ground, whereupon Burke knelt or sat on their chests, expelling the air and interfering with inspiratory efforts. He then put one hand over the victim’s nose and mouth and used the other hand to press the lower jaw towards the upper. Suffocating Gases Deaths from suffocating gases are caused, not by the toxic nature of the gases, but rather by displacement of oxygen from the atmosphere. Carbon dioxide and methane are the two most commonly encountered suffocating gases. Methane is the principal constituent (94–96%) of natural gas that is used for cooking. It is odorless; the smell we detect from natural gas is an added ingredient to make leaks detectable. Reduction of atmospheric oxygen to less than 25% of normal (5–6% by volume of oxygen) by displacement of oxygen by inert gases, such as carbon dioxide and methane, produces uncon- sciousness in seconds and death in a matter of minutes. Determination of the cause of death in such cases is by knowledge of the circumstances sur- rounding the death. Toxicological analysis of the blood is of no help in the case of carbon dioxide, because it Asphyxia 245 is a normal constituent of blood. Since the gas is not toxic, however, all that its identification would indicate is that the individual was exposed to an atmosphere containing methane, not that death was due to it. Strangulation Strangulation is a form of asphyxia characterized by closure of the blood vessels and air passages of the neck as a result of external pressure on the neck. Manual strangulation Virtually all hangings are suicide and all ligature and manual strangula- tions homicide. In the last ten years, murders ascribed to strangulation have averaged 286 a year, with a range of 366 to 211. The increase would be minor, as the total number of homicides ascribed to just asphyxiation in that same time period averaged 107 a year.
Purchase 250 mcg seroflo. How to Keep Pollen Allergens Outside.
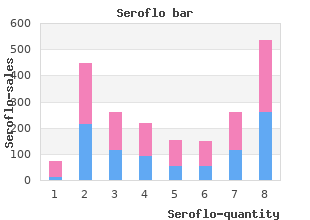
In developed countries the indoor level of most air pollutants is often lower than purchase seroflo 250mcg mastercard allergy medicine 7 year program, but highly correlated with order generic seroflo on line allergy treatment new, their outdoor concentration generic 250 mcg seroflo overnight delivery allergy treatment melbourne. Air Pollution and Cardiovascular Mortality Data from the first longitudinal cohort studies showed that the adjusted mortality rate ratio of the most polluted to the least polluted cities was 1. Air pollution was positively associated with deaths from lung cancer and cardiopulmonary disease. In Europe, outdoor pollution was found to be responsible for 6% of total mortality, half of which could be attributed to automobile emission. Interestingly, the number of deaths attributable to air pollution exceeded that from motor vehicle crashes. This impact is comparable or greater than estimates for secondhand smoke exposure. In Europe, exposure to biomass smoke has been linked to 40,000 premature deaths per year. Most such effects have been linked to particulate air pollution, which is a readily measured constituent of air pollution. Airborne particles inhaled from the ambient air are deposited in the lung or transported in the circulation, where they induce oxidative stress and establish a state of mild inflammation. These alterations manifest as worsening of peripheral artery disease, heart failure, and arrhythmic events and can precipitate acute myocardial infarction or sudden cardiac death. Arrhythmogenesis Exposure to both ambient air pollution and traffic-related pollutants is associated with cardiac electrical instability, alterations in heart rate, and heart rate variability (see Chapters 37 to 39). Similarly, chronic exposure to indoor air pollution can lead to electrical perturbations that may increase arrhythmia risk. Although healthy individuals may be somewhat impervious to the arrhythmogenic effects of air pollution exposure, individuals with preexisting disease are likely to be more sensitive. Exposure to particulate air pollution can affect the autonomic nervous system, often leading to a decrease in parasympathetic tone (see Chapter 99). Ventricular repolarization may also be affected on exposure to household wood smoke. The incremental risk of air pollution in triggering arrhythmias may be higher in elderly persons or individuals who have underlying cardiac disease. Direct effects of chronic exposure to air pollution on cardiac function and remodeling have been reported in both human and animal studies. Chronic exposure to elevated levels of air pollution may lead to the onset of hypertension. Individuals who live near major roadways and are therefore exposed recurrently to traffic-generated pollutants have a higher prevalence of hypertension. Comparing those who live less than 100 m of a major roadway with those who live more than 1000 m, a 9% higher prevalence has been reported. Fine particles are deposited in lung, especially in the alveoli, through sedimentation and brownian diffusion and can also pass into the systemic circulation. These particles carry little or no biologic material and are deposited in the lung in greater quantities than larger particles. In the alveolar spaces, fine particles initially impact the surfactant- rich alveolar lining layer. In addition, impaired surfactant function could lead to chronic lower airway inflammation. The ultrafine particles are mainly deposited in the lung by brownian motion and can pass from the lung to other peripheral organs, including the heart and the brain. The semiquinone-like radicals are chemisorbed on the particles and provide persistent redox-active surfaces of the particles that, in the presence of oxygen, undergo autocatalysis to generate free radicals such as superoxide. Increased production of cytokines in the lung promotes the accumulation of neutrophils, protein and fibrinogen in the bronchoalveolar fluid. For instance, even in normal adult humans, exposure to air pollutants such as diesel exhaust elicits an inflammatory response in the lungs. Occupational Exposures In addition to exposures at home, outside, and in traffic, many individuals are exposed to air pollution at 6 work. Plant workers involved in the synthesis of aldehydes such as formaldehyde, undertakers, embalmers, and perfumery workers reportedly have a higher risk of atherosclerotic heart disease, presumably from recurrent exposure to volatile aldehydes. Experimental studies with animals have substantiated that exposure to 1,3-butadiene can have atherogenic effects. Benzene exposure leads to arrhythmogenesis in animals, and workers exposed to benzene show increased prevalence of arterial hypertension, conduction defects, and repolarization disturbances. Air pollution can also affect workers in occupations that involve frequent exposure to fire and smoke, 15 such as firefighters and military personnel. Management and Intervention Because it is a community-wide problem, air pollution exposure is difficult to control at an individual level. Clearly, the well-established link between air pollution and heart disease should spur and support regulations limiting industrial emissions and traffic. Individual initiative may be particularly important in minimizing exposure to indoor air pollution. In developing countries, indoor air pollution can be drastically reduced by discontinuing the use of solid biomass for fuel or by using chimney woodstoves that prevent the accumulation of indoor air particulates. In developed countries, exposure to particles generated by cooking and frying can be minimized by proper ventilation or filtration. Proper indoor air filtration improves endothelial and microvascular function and may decrease systemic inflammation, even in asymptomatic individuals. Gaseous pollutants are difficult to remove, but most airborne particles can be removed by an electrostatic precipitator in a single-pass efficiency of 90% or greater, even for smaller particles. Similarly, in-vehicle air conditioning can reduce exposure to traffic-generated air pollutants. Lastly, although some dietary interventions have been shown to be marginally effective in decreasing the effects of air pollution, more extensive research is required before such recommendations can be widely advocated or adopted. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Particulate matter air pollution and cardiovascular disease: an update to the scientific statement from the American Heart Association. Coronary heart disease and household air pollution from use of solid fuel: a systematic review. Exposure to fine particulate air pollution causes vascular insulin resistance by inducing pulmonary oxidative stress. Episodic exposure to fine particulate air pollution decreases circulating levels of endothelial progenitor cells. Insulin sensitizers prevent fine particulate matter–induced vascular insulin resistance and changes in endothelial progenitor cell homeostasis. The goal is to help clinicians evaluate symptoms produced by exercise, manage questions and clinical problems in athletes and physically active people, and assess the risks and benefits of exercise for individual patients. Historical Perspective Debate has long surrounded the cardiovascular risks and benefits of exercise. Sky equated the Oxford-Cambridge crew race to cruelty to animals and opined that such extreme 1 exertion would cause heart disease. Evaluation of these normal adaptations by auscultation and cardiac percussion, the diagnostic tests of the day, led to their interpretation as signs of pathologic conduction disease, dilated 1 cardiomyopathy, and valvular obstruction, respectively.
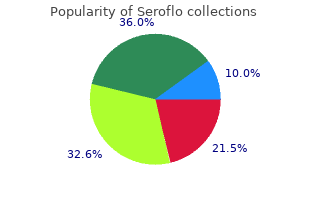
A severe contusion can progress to a delayed perforation several hours or days after injury seroflo 250mcg discount allergy count houston. Transection of the jejunum usually occurs just distal to the ligament of Treitz purchase 250 mcg seroflo overnight delivery allergy symptoms dark circles under eyes, where the jejunum is firmly attached to the posterior abdominal wall cheapest seroflo allergy forecast kentucky. In transection of the small bowel, there is usually associated injury to the mesentery. Spontaneous rupture of the small bowel may occur due to infarctions secondary to incarceration, strangulation, various ulcer- ative diseases of the mucosa, and thrombosis of the mesenteric vasculature. With severe blunt trauma to the abdomen and injury to internal organs, the mesentery of the small intestine is often contused or torn. The mesentery appears to be torn most often by a tangential blow to the abdomen that exerts traction on the mem- brane. Death could occur solely from injury to the mesentery if there is laceration of one of the large blood vessels coursing through the mesentery. The large intestine differs from the small intestine in its larger caliber, more fixed position and less vulnerability to trauma. The midportion or transverse colon is the most open to trauma because of its relation to the vertebral column and its exposed position in the mid abdominal cavity. A severe impact to the anterior abdominal wall may crush the midportion of the transverse colon between the anterior abdominal wall and the lumbar vertebrae. The resulting traumatic lesion depends on the severity of the blunt force and might range from a contusion to a laceration to transection. Rup- ture of the colon may also occur following insertion of foreign objects, hands, or animals for sexual stimulation. Blunt Trauma Injuries of the Trunk and Extremities 139 Kidneys The kidneys are situated in the posterior part of the abdomen on either side of the vertebral column behind the peritoneum. The posterior surface and upper portion of the right kidney rest on the 12th rib; the left kidney usually rests on the 11th and 12th ribs. The anterior surface of the right kidney is in contact with the right adrenal gland, liver, and the right colic flexure. The anterior surface of the left kidney is in contact with the left adrenal gland, stomach, spleen, jejunum, colon, and, medially, the pancreas. They are usually seen following motor vehicle accidents or falls from great heights when there is massive blunt force trauma to the abdominal cavity. Blunt force applied to the flank may crush the kidney between the abdominal wall and the lumbar vertebrae. Aside from contusions, the major- ity of injuries to the kidney are small transverse lacerations beneath an intact capsule with minimal hemorrhage. Injuries producing massive lacerations of the kidneys up to fragmentation are uncommon and are associated with massive injury to the other abdominal organs. Urinary Bladder In adults, the empty urinary bladder is placed entirely within the pelvis, behind the pubic symphysis. In children, the anterior surface of the bladder is in contact with the lower two-thirds of the abdominal wall between the sym- physis pubis and the umbilicus. Beginning at puberty, it slowly begins to descend to its final position in the pelvis. Iatrogenic rupture of the urinary bladder may occur during instrumentation for diagnostic or therapeutic purposes. More commonly, severe blunt trauma to the pelvis and lower abdomen causes rupture. The degree and type of injury that occurs usually depends on the volume of urine in the bladder. Extraperitoneal occurs when the bladder is empty or contains only a small amount of urine. In extraperitoneal rupture, the bladder lies within the pelvis and is protected by the strong bony pelvis. Here lacerations of the urinary bladder are associated with fractures of the pelvis. This is when blunt force is applied to the lower abdominal wall in a downward direction. Intraperitoneal rupture of the urinary bladder occurs when the bladder is markedly distended by urine. At this time, a kick, a blow, or any blunt force to the lower abdominal wall can compress the posterior wall of the 140 Forensic Pathology bladder against the sacrum, raising the pressure within the bladder lumen and rupturing it, with urine entering the abdominal cavity. When they do occur, they are usually associated with extensive fractures of the pelvis. Blunt trauma injuries to the pregnant uterus and/or fetus are usually caused by automobile accidents, with falls and assaults accounting for a significantly smaller num- ber of cases. Sep- aration occurs at the moment of trauma but may not become evident for a few hours. This is probably due to a small separation at the edge of the placenta, with development of a retroplacental hematoma that takes a while to grow and kill the fetus. In the absence of any direct trauma, the cause for the separation is severe distortion of the uterus that can occur with violent motion. Following the death of the fetus, labor usually begins within 48 h, though it may be delayed up to a few weeks. During this time, the mother may develop a disseminated intravascular coagulopathy. With fractures of the pelvis, there may be not only placental separation but direct fetal injury, for example, fracture of the fetal skull and/or internal injuries to the fetus. Blunt Force Injuries of the Extremities These injuries may be limited to the skin and subcutaneous tissues or extend to muscles, blood vessels, nerves, bones, and joints. Avulsive wounds of the lower extremities are most frequently seen in automobile–pedestrian accidents. If an automobile wheel passes over the lower extremities, it can exert tangential pressure on the skin and subcu- taneous tissues, separating them from the underlying muscles. In other instances, the skin and subcutaneous tissue are also torn, forming a large flap of skin (Figure 5. A blood-filled pocket may also be produced in the back and/or lateral (outer) aspect of the thigh in pedestrians impacted by the front of the hood. The tangential force of the hood impacting the thigh strips the skin and subcutaneous tissue from the muscle, creating a blood-filled pocket (Figure 5. Complications of Blunt Force Injuries to the Lower Extremities Shock — caused by severe crushing, soft tissue injuries, and/or com- pound fracture. Hemorrhage — occurs from traumatic amputation, compound fracture with severing of a large vessel, multiple lacerations, or severe avulsive wounds Blunt Trauma Injuries of the Trunk and Extremities 141 A B C Figure 5. Venous thrombosis with fatal pulmonary embolism — Veins may be injured directly by fracture of the lower extremity, with resultant thrombosis. Thrombosis may also be secondary to venous stasis following prolonged immobilization of the lower extremity when the patient is confined to bed with a fractured extremity. There may be crushing injuries rather than frac- tures of the lower extremity with either direct injury to the veins or stasis bv compressing hemorrhage and edema resulting from the leg injury. Fat embolism — Fat embolism follows mechanical trauma that mobi- lizes the fat from an injured fat deposit in the body.
Comparison of novel risk markers for improvement in cardiovascular risk assessment in intermediate-risk individuals effective seroflo 250 mcg allergy medicine xyzal. Effect of varenicline on smoking cessation through smoking reduction: a randomized clinical trial purchase generic seroflo on line allergy shots ohip. Effects of nicotine patch vs varenicline vs combination nicotine replacement therapy on smoking cessation at 26 weeks: a randomized clinical trial order seroflo 250 mcg amex allergy medicine 180 mg. Increasing prescription length could cut cardiovascular disease burden and produce savings in South Africa. Cardiovascular disease screening by community health workers can be cost-effective in low-resource countries. Community programs for the prevention of cardiovascular disease: a systematic review. While often seen as addressing the distinction between what “can” and what “should” be done in clinical practice, the scope of ethics is much wider, encompassing such diverse topics as genetic testing, appropriateness- based reimbursement policies, and end-of-life decision making. This attests to the awareness that, as technology and science have advanced cardiovascular medicine, so too has the need for ethical reasoning and clinically nuanced discussions of ethical challenges. This chapter focuses on categories within cardiovascular medicine that highlight the need for ethical reasoning: informed consent and decision aids, clinical ethical judgments of futility, conflicts of interest and disclosure, public reporting, social media and mobile health, genetics, and transplantation. Informed Consent and Decision Aids One general approach to ethical reasoning is that of principlism, deploying the ethical principles, or guides for clinical ethical judgment and action, of respect for autonomy, beneficence, nonmaleficence, and justice. As a consequence, respect for autonomy is often regarded as the most important ethical principle. The nuances of the conversations that should take place with patients are difficult to master for clinicians and can become time-consuming when caring for patients with complex heart disease but are often relegated to junior staff or extenders. The goal of informed consent is to empower the patient with clinical information relevant to the decision at hand and to support the patient in making a voluntary decision, that is, a decision free of controlling internal influences (e. What constitutes “relevant facts” was established with the “reasonable patient standard” in the 1972 Canterbury v. This standard requires the physician to provide information that any patient with a specific condition, such as stage C heart failure, needs to know. This is a patient-oriented standard and is the legal standard in the majority of the states in the United States. Although the accepted legal and ethical standard of practice, informed consent continues to be poorly 4 done and is heavily biased by physician time and preference. The common practice of “discussing” an angiographic finding while a patient is in the cardiac catheterization laboratory and making the decision to intervene is far from ideal; the practical constraints of time often interfere in many settings, as when it would otherwise be reasonable to perform a staged coronary intervention. In some settings, such as emergency care that often includes the presentation of an acute coronary syndrome or aborted sudden death, clinicians practice under the guise of “presumed consent,” and the best interest standard applies to medical care. This standard is based on the ethical principle of beneficence, which creates the ethical obligation to provide clinical management that is expected in evidence-based clinical judgment to result in net clinical benefit for the patient. When patients lack decisional capacity or they are temporarily unable to make decisions, as when sedated, clinicians turn to legally designated surrogate decision makers. Surrogates should act with substituted judgment, making decisions the patient would have made, not necessarily what the surrogates themselves would want or think appropriate. In this situation the process of informed consent often becomes increasingly complicated and time sensitive. The impetus in clinical medicine is to rescue with all tools at hand, whereas the reality may be that rescuing someone from immediate death will only delay more difficult decisions about limiting life-sustaining treatment for only a few days or weeks. This does not mean that no emergency therapies should be performed because of the risk for misunderstanding, but rather that the process of informing patients and their families and updating them with current facts and probable outcomes is iterative. It is often in the setting of informed consent that tension between the principles of respect for patient autonomy and beneficence are most acutely experienced. Clinicians may believe that a particular intervention or medication is clearly superior to the alternative, but the patient may not agree. Because of this tension, the use of decision-making aids has been increasingly adopted within cardiology. Meaningfully informed patients are less likely to undergo procedures that have limited benefit or benefits not consistent with their preferences. Patients who have been meaningfully involved in decisions about their medications are more likely to be compliant with them. In this setting, use of a decision aid is valuable to allow for the time to discuss these issues. Decision aids or other tools are used to address the medical evidence, consider clinical judgment, and integrate patient preferences. Having a legally designated surrogate make the decision, in the absence of any prior discussion of the ramifications of this life-altering implantation, is not recommended, such as in cases of acute precipitous cardiogenic shock. Turning off a device allows the patient to die from the underlying disease process, or malignant arrhythmia when and if it occurs (see Chapter 41). The immediate consequences to the patient and surrogate as well as the clinician are inescapable. One important distinction is that although there are community-dwelling patients who are chronically supported by mechanical ventilation, their numbers are few and their medical condition usually obvious (e. Clinical Ethical Judgments of Futility In general, futility means that in evidence-based clinical judgment, there is no reasonable expectation that a clinical intervention will result in its usual outcome. When this is the case, the beneficence-based obligation to provide clinical management has reached its limits, and discontinuation should be offered. When continuation of futile treatment results in significant iatrogenic or disease-related burden, there is a 14 beneficence-based obligation to recommend that the intervention be discontinued. For this general concept of futility to become clinically applicable, the concepts of “no reasonable 15 expectation” and “outcome” must be specified. Because the invocation of futility sets the clinician and patient on a path to limitation of life-sustaining treatment, the concept of “no reasonable expectation” should be specified conservatively. There are three beneficence-based specifications of “outcome” and one autonomy-based specification that are clinically distinguishable and applicable. The first beneficence-based specification is physiologic outcome: a clinical intervention should be considered physiologically futile when there is no reasonable expectation that its physiologic outcome will occur. The addition of a fifth vasopressor in the setting of critical cardiogenic shock will not reasonably restore cardiac output and can be considered to be physiologically futile. The second beneficence-based specification is the outcome of death during the current admission and no recovery of interactive capacity before death occurs. The third beneficence-based specification is the outcome of survival but with irreversible loss of interactive capacity, such as a permanent vegetative state as determined by American Academy of Neurology 18 criteria. The one autonomy-based specification of the outcome is a functional status that the patient judges to be incompatible with engaging in valued life tasks and deriving satisfaction from doing so. Whenever one or more of these definitions of futility apply to a clinical intervention, the physician should offer discontinuation of that intervention, or importantly in cardiovascular medicine, the physicians should not offer an intervention. Conflicts of Interest and Disclosure The profession of medicine is based on the fiduciary relationship, or “putting the patient first”; the maintenance of scientific competency; and being entrusted with the responsibility to improve the health of the public.
Additional information: